Orange County Meniscus Tear Treatment by Steve Mora MD Orthopedic Surgeon
Hey doc my friend told me that after his meniscus tear surgery he developed arthritis. Because of this I really don’t know if I want surgery on my knee. What do you think?
I get asked questions about meniscus tears and arthritis a dozen times a day. Meniscus tears are the most common problem we see in orthopaedics. It is not uncommon for patients who have meniscus tears to think that by having knee arthroscopy and trimming of the tear (partial meniscectomy) it will increase the chance of arthritis or speed up the onset of arthritis. The idea that knee arthroscopy and partial medial or lateral meniscectomy increases the onset of arthritis is due the idea that during surgery a normal meniscus is removed. I tell them that in the contrary the goal of meniscus surgery is to preserve as much of the normal meniscus as possible.
I like to explain things like this: Your knee pain is most likely being caused by the torn and loose meniscus fragments. Sometimes these fragments irritate the knee and cause it to swell or become inflamed. Due to the fact that these fragments are torn, they no longer properly function as “cushions” or “shock absorbers”. Therefore, the torn pieces of meniscus are for the most part creating problems such as inflammation, mechanical symptoms, i.e. catching, or abrading and damaging the nearby surfaces. The goal of surgery is therefore to trim or repair the torn fragments. Many years ago it was common practice to completely remove a torn meniscus tissue by doing a total meniscectomy. Currently the goal of surgery is to trim back only torn pieces or repair whenever possible. I also tell patients that their arthroscopic partial meniscectomy surgery is in an of itself not changing the natural history of the knee. The tear has changed the course of the knee; not the fact that they had surgery. For example, if a patient has a large non repairable bucket handle meniscus tear, they will probably develop arthritis with or without surgery. The only difference is that by having arthroscopy they will most likely have more comfort and, therefore, be able to do more; improve their function. At the same time if the patient has a repairable tear it will most likely benefit the knee longevity to have it repaired.
I also like to take the time to explain to my patients that meniscus tear patterns occur in different ways. Sometimes the tears look like small hangnails that just require trimming or sometimes they are like rips in the center of a piece of paper that need to be sewn back together. In cases where the pieces are small and hangnail-like, we have an instrument that is very similar to a nail clipper that removes the torn fragments; that is called a partial meniscectomy. If the tear is like a rip in the center of a piece of paper and it can be closed up with sutures we call that a meniscus repair. If a tear can be repaired successfully the meniscus can continue to provide the same shock absorbing function it had before the tear. For this reason we try to repair when possible.
Pictures of Meniscus Tears:
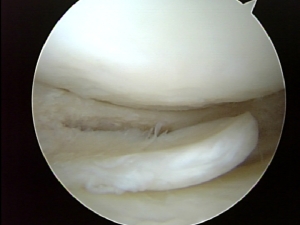 Typical Medial Meniscus tear of the knee. The torn fragments act similar to painful hang nails which can cause pain when shifted or pulled. Patients typically have pain when the fragment moves into a tight area of the knee. The patient will typically report episodic stabbing pain.
Typical Medial Meniscus tear of the knee. The torn fragments act similar to painful hang nails which can cause pain when shifted or pulled. Patients typically have pain when the fragment moves into a tight area of the knee. The patient will typically report episodic stabbing pain.
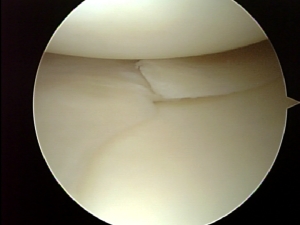 In some cases the torn piece does not move and therefore does not cause much pain.
In some cases the torn piece does not move and therefore does not cause much pain.
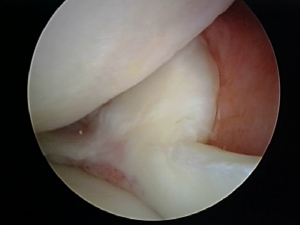 Another picture of a tear that had flipped up and was caught between the joint surface and the capsule
Another picture of a tear that had flipped up and was caught between the joint surface and the capsule
 Another tear which was small but caused significant pain. This tear underwent trimming.
Another tear which was small but caused significant pain. This tear underwent trimming.
 This surgical picture shows a medial meniscus tear which underwent partial medial meniscectomy (trimming)
This surgical picture shows a medial meniscus tear which underwent partial medial meniscectomy (trimming)
 Example of a “Bucket handle” meniscus tear. The best way to describe this tear is to compare it to a rip in the center of a cloth. It might be repairable be stitching it back together.
Example of a “Bucket handle” meniscus tear. The best way to describe this tear is to compare it to a rip in the center of a cloth. It might be repairable be stitching it back together.
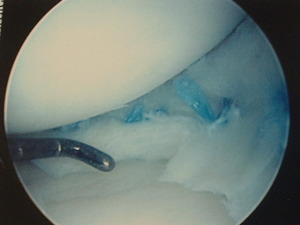 Repair of the bucket handle meniscus tear with multiple meniscus sutures. The goal of the surgery is to create a healing environment by creating a bleeding response and firmly suturing the edges together.
Repair of the bucket handle meniscus tear with multiple meniscus sutures. The goal of the surgery is to create a healing environment by creating a bleeding response and firmly suturing the edges together.
The only reason we would not repair a torn meniscus is if the pattern does not allow, the pieces are too shredded and cannot hold the sutures or the tear is in a non vascular zone.
The main difference between between the 2 types of tears is that in one case I am trimming the small torn pieces (partial meniscectomy) and in the other case I am closing up the tear with sutures (repair). As mentioned above, my goal as your orthopaedic surgeon is to preserve as much normal meniscus tissue as possible and/or repair whenever possible.
The length of time required with crutches is 1-2 weeks after partial meniscectomy. If the tear is repaired, then I remind the patients that their knee needs to be “babied” or “protected” to allow the tear to seal itself, i.e. to heal. If the knee is moved in the wrong manner the small sutures can be ripped out. Once it is described in this manner my patients completely understand and accept why they might have to use crutches or a brace for up to 6 weeks after meniscus repair.
I hope this information regarding meniscus tear treatment and the development of arthritis is helpful. Thank you for taking the time.
Dr. Mora is a native of Orange County. He graduated from Anaheim High School in Orange County CA. He completed his training at the UC Irvine where he finished in the top of his class with AOA Medical Society honors. He completed his Orthopedic Surgery training USC. He completed an extra year of training with a Sports Medicine, Cartilage, Shoulder, and Knee Fellowship at Santa Monica Orthopaedic and Sports Medicine Group. He is currently practicing Orthopaedic Surgery in Orange County and is on staff at St. Joseph Hospital in Orange. Dr. Mora’s practice focus is on sports related trauma, knee ligament and cartilage repair, shoulder rotator cuff and instability, hip arthroscopy and Makoplasty partial knee replacement. He sees athletes of all levels including professional soccer and UFC/MMA athletes. He is team doctor for the Anaheim Bolts pro indoor soccer team and Foothill High School. Dr. Mora performs Cartilage transplantation (Genzyme), partial custom knee replacement, OATS, tibial osteotomies, meniscus transplant, shoulder Laterjet procedure, shoulder replacement, elbow arthroscopy, PRP and adult stem cell injections and hip arthroscopy. Dr. Mora’s family heritage is Peruvian. He speaks fluent Spanish.
[embedyt]http://www.youtube.com/watch?v=Ic6qj-5zdgw&width=400&height=250[/embedyt]
Steve A. Mora, M.D. Orange County Board Certified Orthopaedic Surgeon Fellowship Trained in Sports Medicine Shoulder, Knee, Elbow, and Sports Medicine Specialist Special Interest in MMA and Soccer Injuries.
You can request an appointment with me by calling 714 639-3750 or going to my web page www.MyOrthoDoc.com
DISCLAIMER: The information on this website is provided as a service from our physicians to our patients and the general public. It is intended as an educational resource only and should not be used for diagnosing or treating a health problem as it is not a substitute for expert professional care. If you have or suspect you may have a health problem, please contact us for an appointment, or consult your physician.


