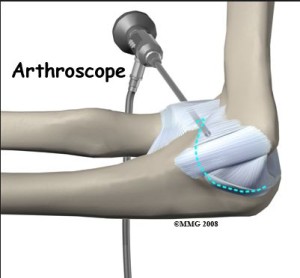
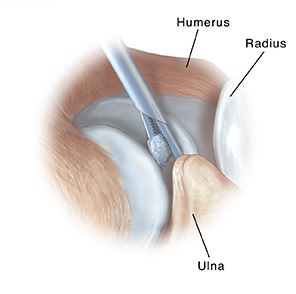
I have been seeing more and more young active patients present with painful and stiff elbow joints. The majority of these patients have been heavily involved in the practice of mixed martial arts (MMA). Most of the ones with severe loss of extension have been professional fighters. It is for this reason that I call this condition “cauliflower elbow”. It is similar to the arthritic elbow we see in older patients but in fighters it occurs at a much younger age.
These patients presented with a stiff and painful elbow that no longer fully straightens out. Since the elbow cannot fully straighten they have problems with reach and with generating a good jab. Patients will eventually decide to seek medical help when the symptoms affect their ability to train at high levels.
Typical Symptoms

-Loss of extension that affects reach or generating a good jab
-Painful catching that will temporarily lock the elbow
-Pain after training that requires more than over the counter medication
-Chronic and severe stiffness that is apparent when the arm dangles, essentially they walk with the arms bent in a un natural manner
The history of the problem is usually one which involves numerous small traumatic events or perhaps a single bad fall onto the mat or an arm bar type of injury (subluxation). Typically the fighter will have taken the usual precautions of resting, icing, anti-inflammatories and immobilization. As time goes on the elbow becomes progressively more stiff. Due to the strenuous training schedule the elbow eventually becomes injured again and again. The stiffness is something that develops over a few months or years. The exact cause of the degeneration is not clear. It is possible that it is from direct impact such as falling onto the mat, elbow strikes, a single trauma such as a subluxation associated with arm bar, or possible due to a traction injury associated with strikes or jabs.
Clinical Findings

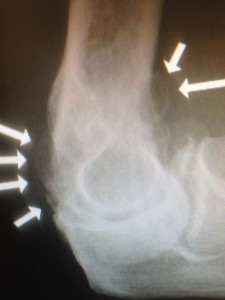
When I examine these fighters they all have various levels of elbow joint tightness and pain. The stiffness is usually with both flexion and extension. Good quality X-rays are very important. They may show anything from a single loose body to advanced degeneration with large spurs, joint narrowing and multiple loose bodies. The loose bodies cause episodic catching. The spurs cause blocks in motion. The degeneration causes pain and tightness. Patients with chronic pain often have profound loss of extension. An MRI or CT is not always required to make the diagnosis. Essentially the diagnosis is made with history, exam and a simple X-ray. A CT scan is good for defining the loose bodies and the spurs. The MRI is good for evaluating edema and the cartilage surfaces.
The Treatment

The treatment of a tight painful elbow depends on various issues: Duration, Severity, Functional deficits, and the presence of loose bodies. Sometimes the pain is from capsular fibrosis (a tight capsule). For example I have had a couple of patients with minimal stiffness but with loose bodies causing painful catching. These patients do well with arthroscopic surgery to simply remove the loose body. However in chronic cases that have tight capsules, spurs and degeneration they require a comprehensive approach that addresses the various pathologies.
The treatment for cases that do not have loose bodies includes: 1-3 Steroid injections into the joint. I also add naturally occurring anti inflammatory called Traumeel and a short course of oral anti-inflammatories such as Celbrex or Naprosyn. Physical Therapy is augmented with a very specific elbow stretching program. Sometimes I recommend dynamic splinting with products such as Dynasplint, JAS brace or a custom made removal night splints. The goal in this situation is to reduce pain, swelling and tightness of the capsule.
Patients are instructed to stretch daily and often. As the tissue stretches the load required to maintain the stretched state reduces and the load is easier to handle and hence the load can be sequentially increased to generate greater effectiveness. Biological tissue is viscoelastic, i.e., It will increase in length (creep) with the application of constant load for a prolonged period of time.
The key to effective stretching is: The longer one can maintain the painful stretch position the more effective the exercise. It’s not about the number of times you push the elbow it’s all about the duration of the push. It is a painful process however when progress is being made it can be seen within 4 weeks of diligent treatment. I always tell my patients that pain while stretching is expected and normal.
Surgery
To see a live surgery demostration please go to my youtube.com channel below.
[embedyt]http://www.youtube.com/watch?v=VvdUBM8a6MQ[/embedyt]
If after approximately 3 months there is limited or no progress I will discuss a surgical option and a post operative program.
The goal of the surgery is: Clean up the joint of loose bodies, shave down the spurs causing blocks and release the tight fibrosed capsule. These goals can usually be achieved with elbow arthroscopy. The procedure is done as a outpatient surgery (home same day). The patient is sleep (General Anesthesia). Arthroscopic surgery involves placing a slender camera into the joint and directly visualizing and treating the pathology in all the compartments. By using the slim arthroscopic camera I am able to directly see the inside of the joint and shave down the impinging spurs and remove any loose bodies (house-keeping).
Once the arthroscopic housekeeping is done, I focus on the tight fibrosed capsule. Most of the time I can do a capsular release with the same arthroscopic instruments through the same key-hole incisions made for the housekeeping portion of the procedure. Due to the close proximity of the nerves and arteries that cross the elbow, arthroscopic capsular release is a challenging procedure. The capsule is released so that the elbow joint can reach full motion.
If there were nerve symptoms prior to surgery such as tingling and numbness of the small and ring finger I also plan on doing an ulnar nerve “transposition” . A 4 inch incision is made around the area of the “funny bone”. The nerve is taken out of the groove and placed a bit forward so that it stops getting stretched or damaged in the groove.
Post Op Plan
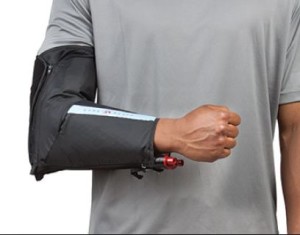
Post operative joint stiffness occurs in phases. It starts with post op bleeding, swelling, granulation tissue formation and later fibrosis. Therefore, the goal after surgery is to control pain, limit swelling and bleeding. To help with recovery after the surgery I recommend taking a short course of a strong anti inflammatory such as indomethacine. When the arm is not being exercised it is kept in the sling only for the first week or two after surgery. A cold therapy unit such as a Game Ready unit is used for the first 2 weeks to control swelling and decrease pain. I will make an extension splint which the patient will use at night to keep the arm straight while sleeping. Night time splinting continues for up to 3-6 months. No one likes sleeping with a hard splint; It is extremely frustrating but important. Physical thereapy with an experience therapist is started a few days after surgery. Once the range of motion is restored the therapist can focus on strength. Good nutrition after surgery is also imperative. I also recommend taking supplements that decrease swelling and improve wound healing. This includes tumeric, glucosamine/chondroitin, arnica, multivitamins, vitamin C, and Zinc.
Summary
I have had success treating combat athletes with this treatment approach. The key to successful treatment is to first recognize that this problem usually worsens unless it is effectively treated. If there is painful catching it is important to look for loose bodies and get them out before they cause further joint damage. It is imperative to address the stiffness when it first starts and not when it is severe. Most early stages of stiffness can be treated without surgery. When it is severe it requires a comprehensive approach that requires surgery and a long rehabilitation period.
About Steve A. Mora MD:
Dr. Mora is a native of Orange County. He graduated from Anaheim High School in Orange County CA. He completed his training at the UC Irvine where he finished in the top of his class with AOA Medical Society honors. He completed his Orthopedic Surgery training USC. He completed an extra year of training with a Sports Medicine, Cartilage, Shoulder, and Knee Fellowship at Santa Monica Orthopaedic and Sports Medical Group. He is currently practicing Orthopedic Surgery in Orange County at Restore Orthopedics and Spine Center.
Dr. Mora’s practice focus on Sports Trauma, Knee Arthroscopy, Shoulder Arthroscopy, Hip Arthroscopy, Elbow Arthroscopy, and Cartilage Restoration of the knee. He sees athletes of all levels including professional soccer and UFC/MMA.
He is team doctor for the Anaheim Bolts pro indoor soccer team and Foothill High School.
Dr. Mora’s family heritage is Peruvian. He speaks fluent Spanish.
[embedyt]http://www.youtube.com/watch?v=Ic6qj-5zdgw&width=400&height=250[/embedyt]
|
Check out my Profile on Yelp
|
For more info become a Fan!
|
Dr. Mora’s Twitter Link: 4000+ Followers
|
My Professional LinkedIn Profile
|
Address:
Restore Orthopedics and Spine Center
112o W. La Veta Ave, Third Floor
Orange, CA 92868
Office: (714) 332-5498
Fax: (714) 941-9539
E-mail: smora@restoreorthopedics.com
Error: Contact form not found.
[slideshow_deploy id=’1142′]